Can the dental sector benefit from AI? How can a Hybrid Classification Model improve Reliability, not just Accuracy?
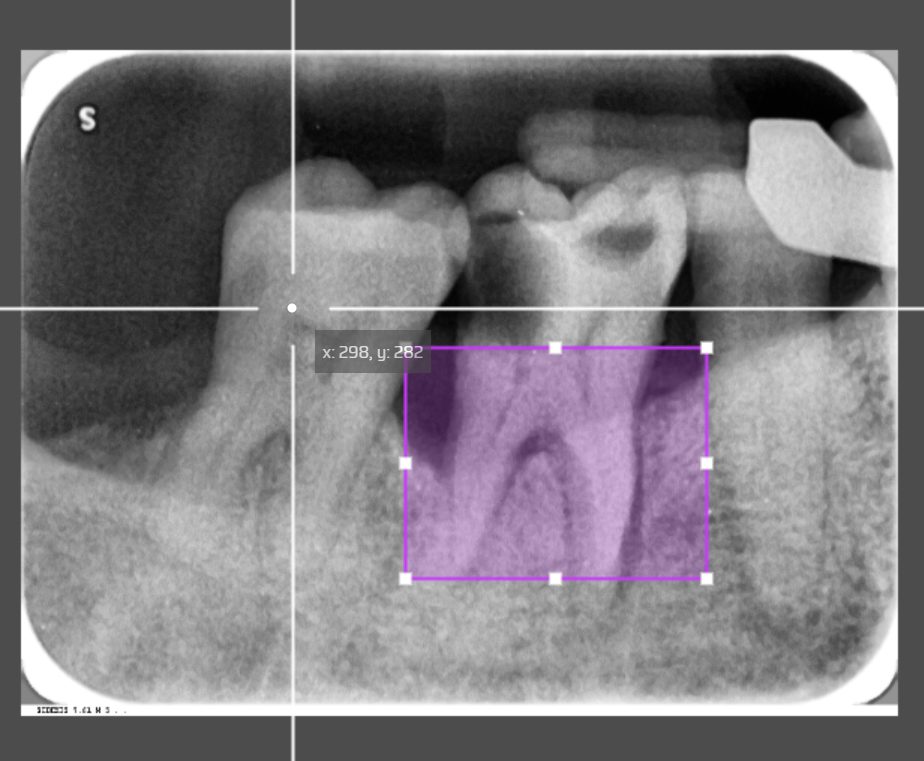
A Hybrid AI model that combines the full X-Ray scope with a critical, detailed area of dentist-based focus can classify periodontal disease with greater reliability.
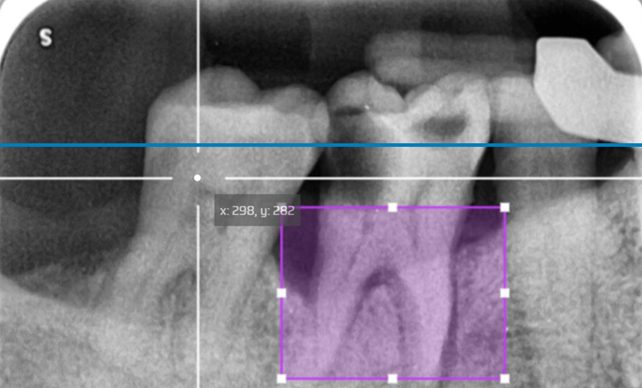
Even though Periodontal disease is not well-known among external workers besides dentists and dental practitioners, the disease is a threat to oral health. While the development of Artificial Intelligence is proceeding quickly, a system that can support these workers by helping them to spot potential issues from the dental radiographs was built. However, feeding the computer with an entire X-Ray image is not ideally effective. If you think about how people examine the X-Ray image, we usually look at a specific area where the issue is and ignore most of the details in the image. The question is: What if we taught an AI to analyze images the same way a dentist does?
The “Full X-Ray limitation.”
Typically, we develop a deep learning model by feeding the entire image data into the system, which is a correct and 100% automated AI approach. The model learns to look at the full picture and makes predictions based on image features.
However, in healthcare, the periapical view of X-Ray images can be complicated, as it contains “noise,” an area of the mouth, teeth, space, and a large number of details that do not have influences towards the results. When the AI tries to analyze a huge amount of irrelevant information, its accuracy is not only declined by paying attention to the wrong place, but the results are not reliable, as the model might learn a shortcut that can be for example, other issues within the dental cavities like caries.
The Effect of the Region of Interest (ROI)
The solution to this was a hybrid classification. Instead of relying 100% on the full image, we introduce a second input data, a cropped highlighted image which simulates the dentist’s analysis area, into the same neural networks. This specific area is the Region of Interest. Then, we apply a scale layer for both inputs with weight fusion. The AI model now relies on
The full image (50%): First input representing the model learn without human intervention, providing the overall context of the patient’s dental cavities.
The cropped ROI (50%): Second input representing the model learn the area created specifically where dentists look within ROI coordinates.
The combined weights: A combination of the full image input and the cropped ROI input for a single prediction.
Better Accuracy, Reliability with Human-AI Collaboration
The outcome of the thesis is that this hybrid approach with half AI and half humanbias increases the accuracy from 78% to 82% while still maintaining reliability more than relying 100% purely on the cropped ROI. Because we handle ROI manually, the dental care professional guides the model by cropping the images for the second input, alongside the deep learning approach.
Full Automation Possibilities
While this hybrid model achieves great accuracy, it requires humans to do the work by cropping the relevant region where the periodontal disease occurs. For future development, we can introduce object detection and object localization to create an automatic disease detection system that crops the full image for the second ROI input by itself.
Future Dental Disease Prediction
The thesis can progress further with extension using Machine Learning approaches to calculate the bone loss percentage within the area after receiving output from the current classification model. This would provide dentists with degrees of disease severity.
References:
Yusufee 2026. Deep Learning–Based ROI Hybrid Classification of Periodontal
Disease in Dental Radiographs: Turku University of Applied Sciences Thesis
Image created with www.makesense.ai